

Dry eye syndrome and blepharitis are common eye conditions that can cause various uncomfortable symptoms. At Virginia Eye Center, our eye doctors have the knowledge and expertise to create a treatment plan to improve your symptoms.
Take our dry-eye self-test to assess your symptoms.
Dry eye syndrome is a common eye condition that can cause various symptoms. Often, dry eye syndrome occurs when your eyes struggle to produce proper tears or maintain the tear film.
The tear film coats the surface of the transparent dome at the front of your eye, known as the cornea. A healthy tear film is vital for a healthy and comfortable cornea. In order for your tear film to be healthy, it must be adequately balanced with the proper amount of each of its components. The three components that make up the tear film are oil, mucus, and water.
The oil layer, also known as the lipid layer, sits the furthest away from your cornea. This layer is responsible for lubrication, and it prevents evaporation.
The water layer is the middle layer and is also known as the aqueous layer. The water layer nourishes and protects the eye.
The mucus layer, also known as the mucin layer, sits closest to the surface of your eye. This layer is responsible for assisting the tears in adhering to your eyes.
When your tear film is well balanced with the appropriate amount of each layer, your cornea stays healthy and lubricated. However, if there is a problem with the production of any one of the layers, your cornea may become dry.
Blepharitis is common and persistent inflammation of the eyelids. Typically, this eye condition occurs when the small glands that produce the oils necessary for the tear film become clogged.
These tiny glands are located along the edge of your eyelid, near your eyelashes. When these glands become clogged, it can cause a variety of symptoms.
Everyone has bacteria on the surface of their skin, but in some people, bacteria thrive in the skin at the base of the eyelashes. For these people, large amounts of bacteria around the eyelashes can cause dandruff-like scales and particles to form along the lashes and eyelid margins.
Typically, blepharitis is associated with dry eye syndrome. Blepharitis can occur in adults or children and may occur due to oily skin or dry eyes.
Not everyone will experience the same symptoms of dry eye syndrome or blepharitis.
However, here are some of the most common symptoms of dry eye:
Another common symptom of dry eye syndrome is excessive tearing. Although this may seem contradictory, sometimes the eye will actually produce excessive tears, which will cause them to overflow and run down your cheek.
When this happens, it is often because your tears are not lubricating your eyes successfully. So instead of staying on your eyes to provide moisturization, they begin to fall.
Subsequently, your eye begins to produce additional tears to make up for the ones that have left the eyes.
The symptoms of blepharitis are very similar to dry eye symptoms. Some of the most common symptoms of blepharitis are:
If you are experiencing the symptoms of dry eye syndrome or blepharitis, visit your eye doctor at Virginia Eye Center for an evaluation. Your eye doctor will be able to develop a treatment plan so you can feel better.
The eye doctors at Virginia Eye Center use a variety of treatment options to help improve your dry eye and blepharitis symptoms. Often, they will start treatment by asking you to increase your use of artificial tears.
They may also ask you to make some minor lifestyle changes, like adding a humidifier, blinking more frequently when you’re looking at screens, doing warm compresses, or doing lid scrubs. In some cases, these minor lifestyle changes may not adequately address your symptoms.
At Virginia Eye Center, our eye doctors offer Lipiflow and BlephEx which are in-office procedures to help improve your symptoms.
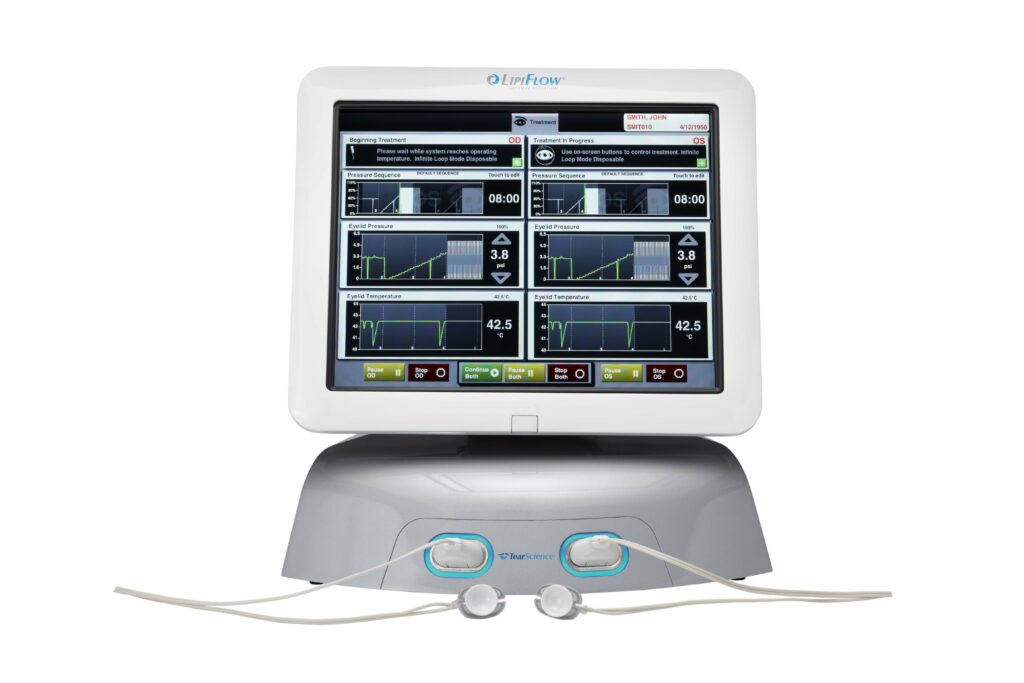
Lipiflow is an in-office treatment that may help improve symptoms of meibomian gland dysfunction and dry eye syndrome. This treatment aims to improve the production of oils necessary for a healthy tear film.
For those who have meibomian gland dysfunction, the glands that produce oils are clogged. During this quick and easy procedure, your eye doctor will place a device on your eyelids, which will provide gentle warmth and massage.
The process of warming and massaging your eyelids helps move any clogged or blocked oils inside the meibomian glands. Although it may take more than one treatment to get the most out of LipiFlow therapy, you will likely notice an improvement in your dry eye symptoms after your first treatment.
BlephEx is a new, in-office procedure that provides unique exfoliation along your eyelids to completely remove the build-up of bacteria and debris that is causing, or will cause, inflammation of your eyelids. This procedure is comparable to getting your teeth cleaned at the dentist.
This deep cleaning treatment will require maintenance at home using eyelid scrubs or warm compresses in between treatments. The procedure takes about thirty minutes to complete.
Are you experiencing symptoms of dry eye or blepharitis? Schedule an appointment at Virginia Eye Center in Leesburg, VA, today!

Sarah Merrill, MD
General Opthalmology, Botox, Cataract Surgery

Soo Shin, MD
General Ophthalmology & Corneal Diseases

Ruby Parikh, M.D.
General Ophthalmology, Cataract Surgery & Uveitis

Christina Chang, MD
General Ophthalmology, Cataract Surgery, Botox

Dana Schneider, M.D.
General Ophthalmology, Cataract Surgery, Corneal Diseases

Elaine Bourdeau, OD
Optometry, Contact Lenses